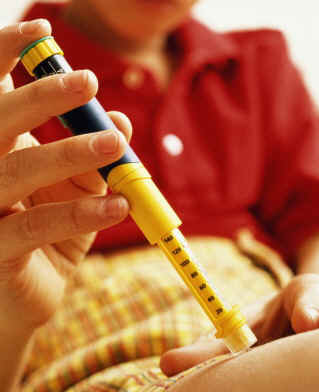
SICK
DAY RULES
And Insulin adjustments during illness
Provided by the Diabetes specialist nursing service Hull and East Yorkshire NHS hospitals trust (last updated June 2001).
- Monitor your blood sugar level at least four times a day.
- Test your urine for ketone levels at every void. If you have moderate to large ketones contact the diabetes nurses or your GP.
- If your blood sugar level is above 13mmol your insulin dose will need increasing as follows:-
- If blood sugar level is 13-17mmol - Take an extra 2 units at each injection.
- If blood sugar level is 17-22mmol - Take an extra 4 units at each injection.
If blood sugar level is above 22mmol - Take an extra 6 units at each injection.
- NEVER STOP TAKING YOUR INSULIN - Even if you are not eating
- Drink plenty of sugar free fluids - approximately 5 pints a day.
- If you are feeling sickly and cannot eat replace food with a sugary fluid, e.g. Lucozade, ordinary fizzy drinks, fresh orange juice etc.
- If you have been sick more than once you must see your doctor for advice.
- Rest - Exercise makes ketoacidosis worse
Why are sick day rules important?
Infection is a precipitating factor in many cases of DKA and HHNS. These are serious life threatening complications of hyperglycaemia. Precipitating factors have previously been discussed on the complications page and it is thought that infection is one of the most common causes. Often patients presenting with DKA and HHNS have been previously undiagnosed until they suffer an infection that triggers off the acute complication (Chiasson et al 2003, Kitabchi et al 2001). Other precipitating factors identified can be trauma, myocardial infarction, cerebrovascular accident, and acute pancreatitis. So it becomes clear that illness plays an important part in the development of these acute complication (Chaisson et al 2003).
Why does illness precipitate some episodes of DKA and HHNS?
Acute physiological stress can cause hyperglycaemia even in non diabetic patients (Quinn 1998, Surwit et al 1992, Kitabchi et al. 2001). When the body suffers from an insult, be it trauma, acute infection, burns or organ failure the body has several protective mechanisms that initiate metabolic and physiological changes. These changes are designed to support the individual through the adverse event. (Edwards 2002). These mechanisms are the inflammatory immune response (IIR) and the neuroendocrine response (NR). They have an immediate impact on the patient. They trigger counter-regulatory hormones (CRH) that attempt to provide the body with the fuel it needs to overcome the adverse event. Glucagon - a CRH - releases stores of glucose from the liver in to the blood stream to provide the much needed fuel. When these stores are exhausted the body begins to catabolise its proteins and lipids. In the individual without diabetes there is usually enough circulating insulin to utilise the glucose in the blood. In diabetic individuals they are unable to use the extra fuel for want of, or resistance to insulin.
However CRH also have a role in causing peripheral resistance to the action of insulin. If the injury or infection is severe or sustained as it is in sepsis for example then the CRH could cause a resistance to insulin in a previously not suffering from diabetes mellitus.
Therefore it is necessary to monitor blood glucose regularly not only of diabetic patients during illness but also of those critically ill patient that may be at risk from hyperglycaemia.
| © | web content copyright © Helen Morgan 2003 |
| web design and code © 56kb.com 2003 |